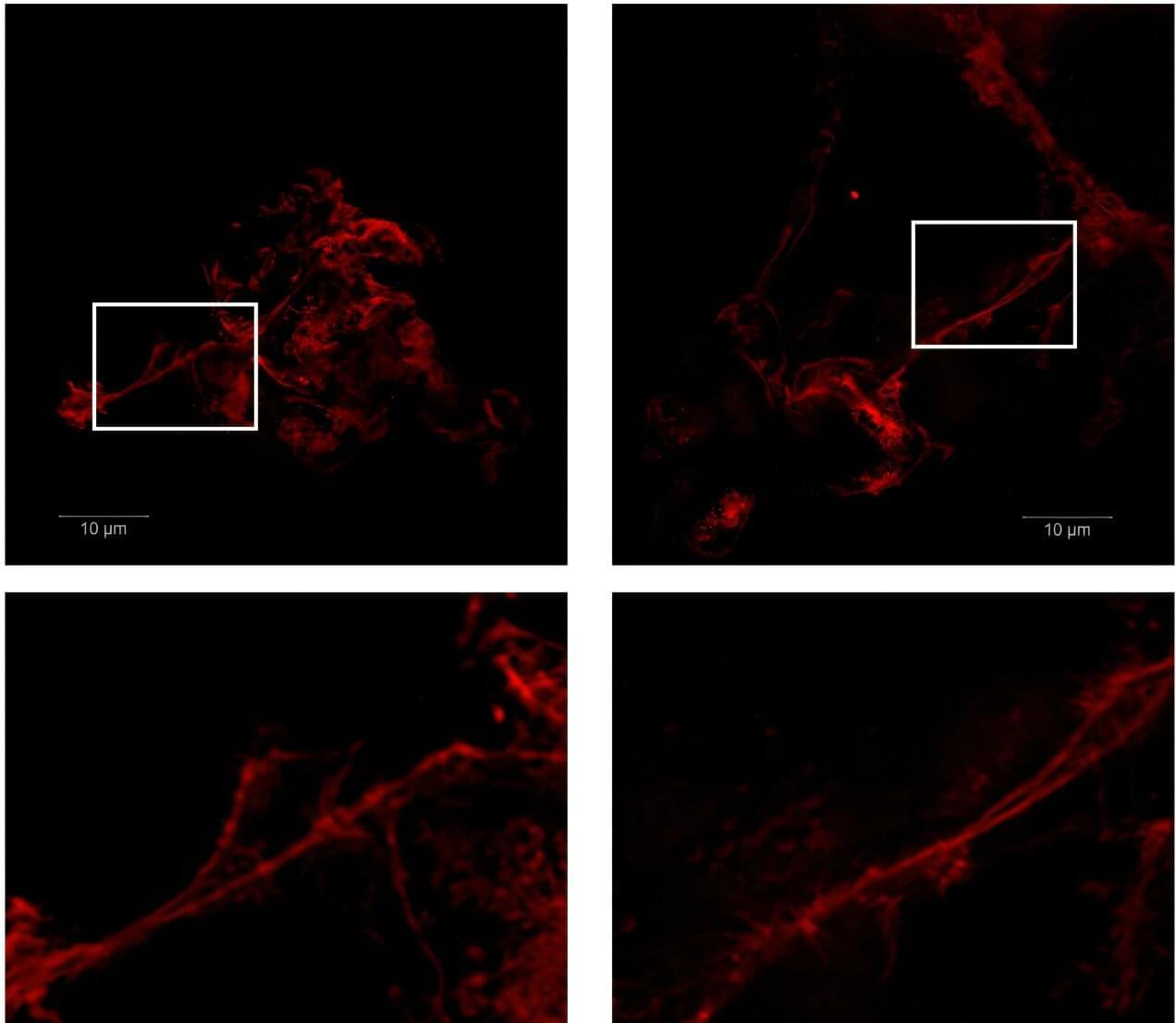
Brain vasculature in ischemic stroke.
Ischemic stroke induces dynamic cellular structural changes in the neurovascular unit, leading to disrupted structural integrity of the blood–brain barrier, neuronal degeneration, and responsive angiogenesis coordinated by endothelial cells, reactive astrocytes, and pericytes.
After ischemic stroke, the neurovascular coupling function of the neurovascular unit is also disrupted, manifested by the metabolic dysregulation of glucose, lipid/fatty acid, and amino acids.
Neurovascular unit dynamic structural remodeling and metabolic dysfunction following ischemic stroke show cellular states and spatiotemporal heterogeneities, revealing new perspectives on ischemic stroke pathogenesis and future therapeutic strategies.
Multidimensional approach aiming to repair neurovascular unit structural disorganization and restore metabolic homeostasis with cellular and spatiotemporal precision is the optimal therapeutic strategy for ischemic stroke. sciencenewshighlights ScienceMission https://sciencemission.com/neurovascular-unit-in-ischemia
The neurovascular unit (NVU) is a multicellular system functioning to maintain healthy brain homeostasis and regulate the exchange of essential elements between the blood and the brain. Recent studies have shown that, in response to ischemic stroke (IS), the NVU undergoes dynamic structural remodeling and metabolic dysfunction, revealing new features of IS pathogenesis. Recent breakthroughs in single-cell multiomics provide emerging evidence regarding the spatiotemporal heterogeneity of NVU responses to IS. To date, clinical treatments for IS-induced brain injury remain very limited. These new studies have advanced our knowledge of the dynamic cellular and molecular changes of the NVU after IS, paving the way for new therapeutic strategies.